- May 2, 2019
- Posted by: Daniel Ryan
- Categories: Foot and Ankle Injuries, Gym Training, Move Physiotherapy

Shin Splints | The Definitive Guide
It seems to be the most well known lower leg condition out there. I feel like everyone either has, or has had them, or knows someone who has suffered with shin splints. With winter sports in full swing, more people are coming into the clinic with this complaint.
Shin Splints has an official name: Medial/Posterior Tibial Stress Syndrome. It is usually a diffuse pain that occurs along the lower third of the shin bone and expands around 5cm.
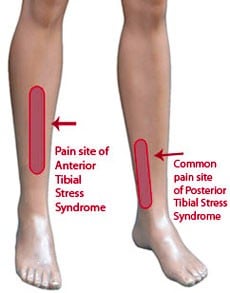
- Shin Splints are the most commonly diagnosed musculoskeletal injury in runners.
- Its reported incidence varies depending on the population group, but it is said to effect between 4 and 19% of the athletic population and 4 to 35% of the military population. 13% to 20% of runners are affected (sprinters, middle and long distance runners).
- It is also suggested that 9.5% of runners are currently experiencing this pain, and up to 20% of dancers are currently affected!
There are two main theories that explain the pain associated with this condition:
- Chronic strain and overuse of the calf muscles results in micro-trauma of the muscles along the inside border of the shin bone.
- Repetitive strain of the calf muscles results in a deep inflammation in the periosteum, a connective tissue layer that covers the shin bone.
It is most common with running and jumping athletes who overload their muscles due to too-faster increases in distance, training intensity and duration. Women are more commonly affected compared to men due to nutritional, hormonal and bio-mechanical differences. Individuals who are overweight are also more susceptible.
Clinical Presentation
Pain will be localised to the inner portion of the shin bone, generally in the middle to lower third. This pain is often experienced in both legs, although this may be to varying degrees.
In mild cases, it is most common for people to experience pain at the start of their run which soon dissipates, only for this pain to return during their cool down. As this condition progresses, it can remain during exercise and be present for hours and days following the activity.
An X-Ray or MRI will show a mild thickening of the periosteum surrounding the tibia in chronic cases; however these scans are often given only to rule out more sinister diagnoses such as stress fractures.
Diagnosis and Examination
Lohrer et al. 2018, highlights an almost algorithmic approach for the diagnosis of MTSS compared to other shin pain pathologies:
- Pain at rest and palpable tenderness can indicate bone stress injuries, including shin splints but also stress fractures.
- No pain at rest with palpable tenderness along the lower leg may indicate a nerve entrapment syndrome.
- No pain at rest, with no palpable tenderness makes chronic exertional compartment syndrome more likely.
However, the caveat here, is for this differential diagnosis, be examined by your physiotherapist. People may think that there are no areas of tenderness along their calf/inner leg and may assume a nerve entrapment or compartment syndrome. But more often than not, your physiotherapist will press on a few trigger points through the inner calf and reproduce that person’s pain almost immediately.
However, in our examination we also want to determine ‘why’ your calf muscles are suddenly becoming tight and overused. This may simply be related to too-faster increases in training load, however more often than not, other biomechanical factors are also at play, including:
- Flat or excessively high arches through your feet.
- Ankle mobility restrictions
- Imbalance between your hamstring and gluteal muscles as compared to your quadriceps muscles.
- Decreased core and pelvic stability during running.
- Leg length discrepancy.
Management
Okay, here is the most important part!
Complete Rest or Activity Modification
Firstly, most people have probably already tried to simply rest. It is most common that people rest and their pain goes away, only for it to return once they start running and training again. And, nobody wins here! In mild cases, complete rest is often not required. However, it may be necessary if your symptoms have progressed to the point of almost constant pain which is present even the day after exercise. Anti-inflammatories and ice packs can help for short-term symptom relief.
However, most rehab plans do require training modification. We need you to change or decrease your training load so that your pain levels are LOW. This means, only 1-2/10 at a maximum during all phases of exercise and following exercise. There should be no pain the next day.
As a general guide, I recommend people either return to their last known pain-free training load. If this amount of training is pain-free, this becomes your new baseline with slow and controlled increases in training load being made from this point. If you do not know your last pain-free training load, start by cutting your training by 50% and start there.
Remember that this only applies to high load situations. So, instead of going mentally crazy by cutting your exercise completely, replace your running sessions with low impact sessions such as swimming, using the cross trainer or resistance training.
Fix Your Biomechanics
This is where your physiotherapist can help the most. Instead of trying to fix everything all at once, your physiotherapist can give you the most effective strategies and targeted areas to treat to get you out of your pain. For the majority of the population, the main biomechanical factor that needs to be addressed is over-pronation during the running cycle – i.e. your foot arch collapsing as you land on it.
In the short-term, orthotics and special arch support taping can address this issue, but of course we are looking for the long term solution. Here are the main factors that contribute to over-pronation:
- Tight Calves: Calf tightness reduces the amount of ankle dorsiflexion (how much your knee can move forwards over your ankle). This means that during the walking and running cycle we must compensate by getting sub-talar movement – which means that our foot flattens. As our foot flattens, the lower leg internally rotates, the knee collapses and the hip internally rotates. It creates a whole chain reaction! The whole effect is a greater amount of loading applied through the inner calf muscles. To release your calves, use a foam roller 2x/daily. Your physiotherapist may utilise massage, dry needling or a home exercise program to address this tightness.
- Proximal Weakness: Just try performing a single leg squat. As most people get to the hardest part of the squat most people will feel their knee collapse inwards. As this knee collapses inwards notice how your foot flattens, overloading the inner calf.Maintaining the stability of the knee is the responsibility of your gluteal muscles, and if your knee does collapse inwards during this movement, it often indicates a weakness. Biomechanically, if this is an issue, this it is also highly obvious when observing people when running hills or climbing steps and stairs. Our Exercise Library page has a number of glute and hamstring strengthening exercises listed that can help with this proximal weakness.
Fix Your Weaknesses
We have already spoken about how gluteal weakness can impact your biomechanics and may require strengthening. (We offer supervised exercise rehabilitation sessions in house at Move Physiotherapy). But what other weaknesses can contribute to Shin Splints?
Calf Weakness
Your calves may be tight, or are they simply weak? Let’s put them to the test, how many single leg calf raises can you do?
- 10-reps: This indicates weakness. Simply going for a run may be over-stressing your calf muscles and causing you pain.
- 20 reps: This is about average, and I would suggest looking elsewhere initially as the cause of your pain.
- 30 reps: Long-distance and ultra-long distance runners should be able to achieve this mark.
If you are finding there is a muscle weakness issue, the best evidence would suggest a strengthening program targeting these areas 3x weekly. You will generally notice your strength improving and symptoms improving within 4-6 weeks.
Work On Your Balance and Control
Finally, how is your balance and control? Just try standing on one leg for 30-seconds. Or better yet, try standing on one leg for 30-seconds with your eyes closed. How did you fare?
As we are running, we spend the majority of our time standing on one leg. Yet, if we can’t control being on one leg standing still, how can we expect to have this level of control during running? As you are standing on one leg at the moment, notice your foot rolling inwards as you lose your control. Now imagine this happening 10,000 times with more load as you land from your stride during your run. This decreased control is a significant contributing factor to a whole host of lower limb injuries, such as patellofemoral knee pain and plantar fasciitis.
Conclusion
A wealth of information (this guide included) exists on the internet about Shin Splints. But your rehabilitation comes down to 3 main factors:
- Rest and activity modification.
- Address your biomechanics – with orthotics, taping, and a specific strengthening protocol.
- Gradually re-load your calves to return to your usual exercise routine, ensuring that you remain pain-free during your training.
If you have read the research and are still struggling, come in for an assessment. Troughout your initial consultation we will give you an exact diagnosis, and outline all of the contributing factors that are playing into your condition. With this information, we WILL get you out of your pain.
